RBCs or Red Blood cells; could these be the next game-changer to chemotherapy? We attempt to explain the research that is currently going on at IIT Delhi. This research works on reducing the toxic side effects of chemotherapy. Prof. Neetu Singh leads it from IIT Delhi Centre of Biomedical Engineering. Without further ado, let's dig right in.
In general, most drugs made by chemists are hydrophobic. However, for practical applications, they are asked to make it hydrophilic. When this transition is made, it is required to make some changes in the chemical structure, which often leads to loss of activity of the drug. Technological advancements have addressed this issue of utilizing hydrophobic drugs in humans by using a drug delivery platform.
How can a drug delivery platform be a solution?
When we consume the drugs, it aggregates due to its slightly hydrophobic nature, and the kidney clears it. Due to this clearance the bioavailability is lowered. Today, we are prescribed a drug of which only a certain percent makes it to the required location in the body to perform its task. These synthetic drugs lead to toxicity issues at such higher concentrations and hence, we see various side effects of the drug in patients. This issue needed to be addressed in order to provide a better less toxic therapy. A drug delivery platform increases the probability of the drug reaching a target site by increasing its circulation in the body for longer duration of time, instead of being identified as a foreign body consequently being thrown out. With the increase in the probability of the drug reaching the desired location in the body, we can now reduce the overall quantity and concentration of the drug being prescribed. An increased effective percentage of the drugs and reduced overall concentration enable modern therapies to ensure the drugs work effectively without causing permanent or temporary damage to the patient's body. This is equally reassuring for the patients.
What strategies are currently being used?
One example is to conjugate albumin to the drug, and another is to use lipid membrane to encapsulate it. Liposomes, or spherical self-assembled lipid bilayer structures, are the most commonly used delivery platforms. Lipid bilayer in liposomes proved to be an effective partition for the drugs. This has been in clinical practice and in the industry for quite some time. This technology allows the drug to sustain itself in the body for a longer duration. However, even liposomes are not the best material. The body identifies them as a foreign substance and clears them too; however, they still do better than free drugs. Moreover, protein interactions with liposomes once inside the body can effect the assembled structure leading to easy disintegration and low colloidal stability in vivo. Once it disintegrates in the body or is thrown out, we simply take another pill.
What is the dilemma, then?
What's the catch, you may ask? The problem faced by the healthcare industry is that there are no efficient drug delivery platforms for majority of drugs used in chemotherapy. In Layman's language, this means that there is a need for technological advancement in drug delivery, and if designed and used intelligently, can possibly reduce the dosage and side-effects of chemotherapy on an unprecedented level.
With curiosity by your side, it's not a hard nut to crack.
How are liposomes formed? We put natural lipids in water, and then we extrude them. We take bigger particles and force them through smaller pores, and with mechanical pressure during extrusion, they become smaller in size. The body does not differentiate these extruded nanoparticles made of synthetic/natural lipids from natural lipids typically present everywhere in the tissues or organs.
Prof. Neetu said that to look for the best possible solution for drug delivery vehicle, they simply asked themselves," How does nature transport cargoes or deliver important components to various sites in the body?"
RBCs are the top delivery vehicles in the body that transports oxygen. Interestingly, the body does not attack the RBC, and allows it to circulate in the body for a long time. The RBCs can also reach every site in the body.
"We simply wondered? What if we could take the same particle, make it smaller in size and use it the way we synthesize liposomes or other lipid nanoparticles?" said Prof. Neetu Singh.
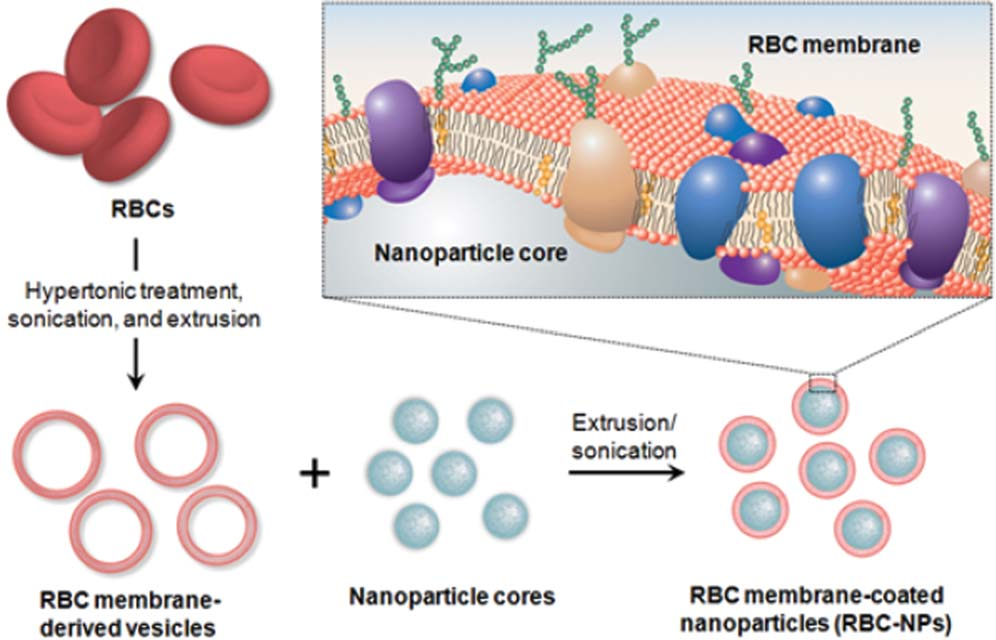
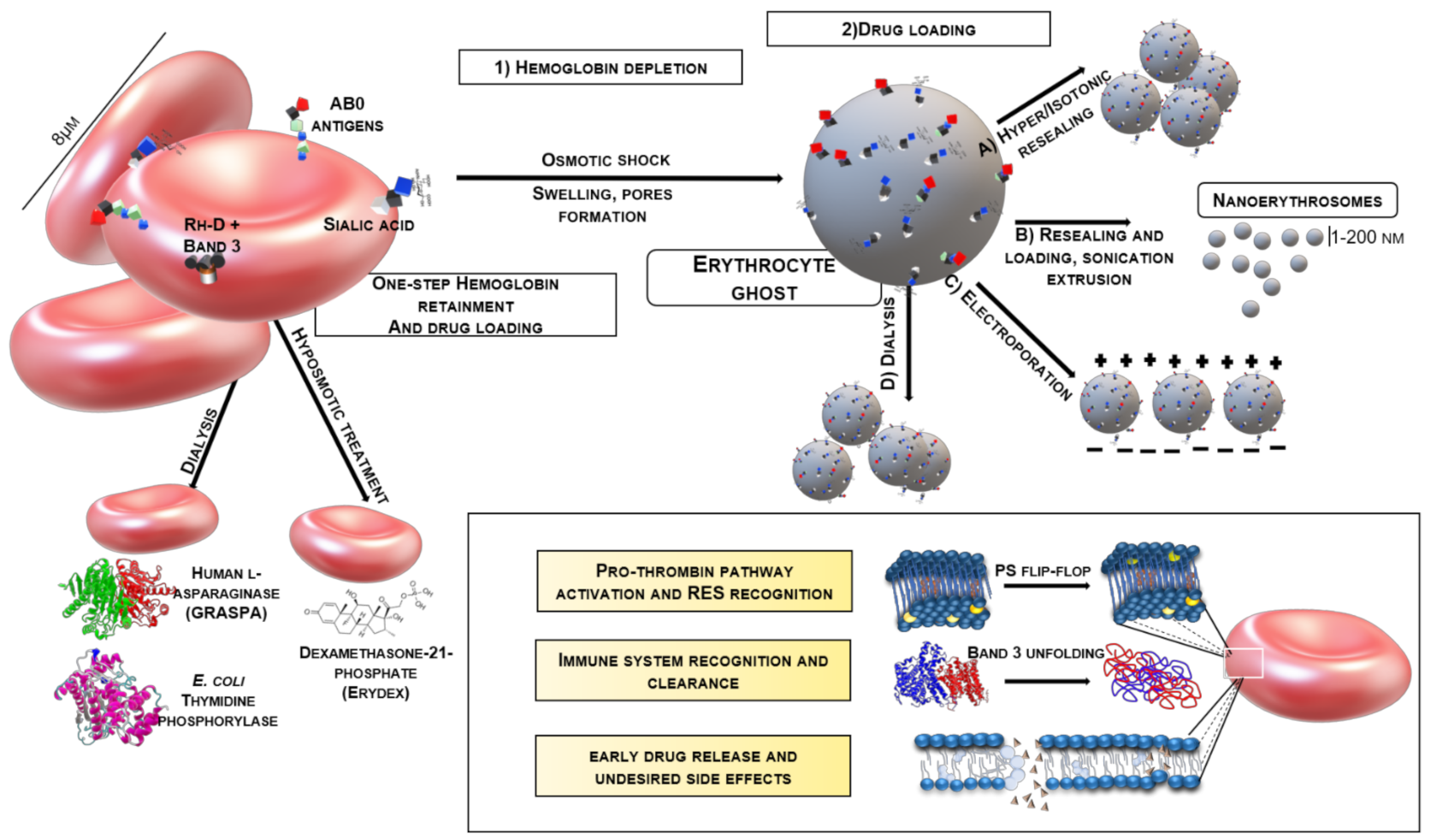
First, the RBCs are emptied and the proteins are removed followed by making them smaller by extruding them. While extruding, if we add hydrophobic drugs dyes and lipid structures, it will assemble with the RBCs lipid membrane. It's now a hybrid structure. This hollow, reassembled and diminished RBC could now be a vehicle for our drugs.
How equipped are we with the knowledge of its implementation?
Prof. Neetu, along with her team, has worked on the comparison between liposomes and RBCs. They hypothesize that the RBCs will be similar to the natural systems and not be cleared by the immune systems.
They still are working on a lot of other challenges. They have very successfully proved that it circulates longer, is more effective and immune system compatible.
When we asked about her inspiration for this journey, she said," We asked very simple questions. Can we replace liposomes with something? We are not biologists; we are naive in that domain of knowledge. We were naive, and that is why we could try it. It's not always good to overanalyze and keep thinking or hypothesizing. One should experiment and learn from experiences too."
To ensure that this technology is biologically safe, they are undertaking in-depth studies to analyze the structre and establish its similarity to natural RBCs with comprehensive protein profiling. They have already established that the key proteins are retained when we extrude the RBCs. Prof. Neetu further explains why she chose to go ahead and try this idea with RBCs and not any other cell of the body. To this, she said," RBCs are made by nature to go through very tight junctions, and this is exactly what we did to them when we extruded them. RBCs are easier to empty out as it has less organelles and no nucleus unlike other cells. As a chemistry person, I very naively started exploiting biological systems using nanochemistry and material science fundamentals, which brought in a new solution, a new perspective."
With technological advancement giving overcoming new stumbling blocks, there is always hope for future developments. Within this ever-evolving world, we live in times of ever-evolving diseases as well. Despite all challenges, humanity has survived through hook and crook and will continue to do so. One of the strong pillars of humanitarian survival is none other than our scientific inclination and of course, the eternal question, "Why?"
With the right proportion of hope, passion and hardwork, humanity has time and again proven itself resilient to change and now with our intelligence will continue to do so.